General Sleep Info:
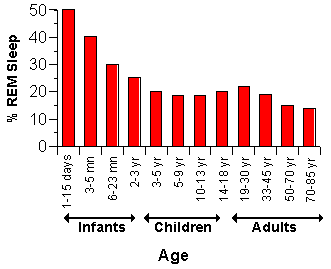
During sleep, we pass through five phases of sleep: stages 1, 2, 3, 4, and REM sleep. NREM Stage 1 is very light sleep; NREM Stage 2 has special brain waves called sleep spindles and K complexes; NREM Stages 3 and 4 show increasingly more high-voltage slow waves. In NREM Stage 4, it is extremely hard to be awakened by external stimuli. The amount of time spent in the deepest stages of NREM (Stages 3 and 4) change from childhood through adulthood. In fact, this change is prominent during adolescence, when about 40 percent of this activity is lost and replaced by Stage 2 NREM sleep. In addition to these changes, the percentage of time spent in REM sleep also changes during development. Adults spend almost 50 percent of their total sleep time in stage 2 sleep, about 20 percent in REM sleep, and the remaining 30 percent in the other stages. Infants, by contrast, spend about half of their sleep time in REM sleep. According to the chart below, a child Jett's age would spend 30% in REM sleep on average.
Sleep in DS:
Although obstructive sleep apnea is seen in only 0.7 to 2 percent of all children, a previous study based on 53 children and adults with Down syndrome between the ages of four weeks and 51 years old (an average of seven years old), found an incidence of sleep abnormalities as high as 100 percent in some cases. George Capone, MD and Director of the Down Syndrome Clinic at Kennedy‐Krieger Institute said in a talk that perhaps poor sleep effects the prefrontal cortex which effects emotions and mental health. 94% of adults with DS had abnormal sleep. 70% had severe OSA (AHI>30/hour) with below 90% oxygen in sleep.
In untreated people with DS, the REM sleep is greatly diminished. Their REM may be in the 2% range. Subjects with DS show a significant reduction in percentage of REM sleep, a marked delay in first REM latency and a statistically significant decrease in high-frequency rapid eye movements during REM sleep. The percentage of REM sleep in humans can be considered as an index of brain "plasticity" and the high-frequency REMs can represent an index of the brain ability to organize information, which is vital for learning and memory.
Also, children with DS show a clearly decreased peak amplitude of growth hormone during sleep; this causes the poor physical development in these subjects and might be related to the occurrence of sleep apnea. Obstructive sleep apnea has also been repeatedly reported in these children; however, if obvious risk factors are absent, children with DS tend to show the presence of central sleep apnea which is caused by a probable dysfunction of autonomic control at a brainstem level.
In people with DS a significant occurance of central, as opposed to obstructive, sleep apneas was found which also showed a significant age-related increase. Central apneas were mostly preceded by sighs, occurred more frequently during sleep stages 1 and REM, and were often organized in long sequences of periodic breathing. Sleep structure was not significantly modified by apneas and oxygen desaturation. It is hypothesized that the increase in central sleep apneas is related to a dysfunction of central respiratory control at the brainstem level in DS (Ferri et al., 1997).
The presence of central sleep apnea induced a further significant increase in low-frequency and very-low-frequency components of heart rate variability, similarly to the effects of the presence of OSA already described in the literature (Schiomi, Guilleminault, Sasanabe, Hirota, Maekawa, et al., 1996).
This final study is additional evidence for impaired brainstem function in DS which is demonstrated by abnormalities in brainstem auditory evoked potentials, abnormal presence of central sleep apnea and impaired balance between sympathetic and vagal control of heart rate variability during sleep.
Finally, the altered balance between the sympathetic and vagal systems can be viewed also in psychophysiological terms, following the ideas of the so-called "Polyvagal Theory" (Porges, 1995) which states that the vagal system does not represent a unitary dimension and is formed by two distinct motor systems. The first one is the "vegetative status" originating in the dorsal motor nucleus, associated with passive automatic regulation of visceral subdiaphragmatic functions, the second is the "smart vagus", originating in the nucleus ambiguus (NA), associated with the active processes of attention, motion, emotion, and communication, with supradiaphragmatic target organs. Thus, the changes reported in the autonomic function of subjects with Down syndrome, together with the already reported changes in central control of respiration (Ferri et al., 1997), might be physiopathologically connected with the basic mechanisms of their developmental psychomotor problems.
Jett's Results:
Sleep summary
The total time in bed was 411.5 minutes. With a total sleep time of 306.5 minutes. Sleep onset latency was 59.5 minutes (The normal time he goes to sleep was an hour after lights out.) with a sleep efficiency of 74.5% (nl>85%). The percentage of sleep time spent in stage N1, N2, N3, and REM was 15.7, 39, 23, and 22.3% respectively with an REM latency of 87 minutes (nl 75-120 minutes). The patient had an arousal index of 10.8 (nl<12) with an arousal awakening index of 10.8 (nl<15). The number of REM awakenings was 0.
Cardiac summary
The average heart rate asleep was 102 bpm. EKG showed normal sinus rhythm.
Respiratory summary
The baseline oxyhemoglobin saturation was 96% with the lowest being 93%. The percentage of sleep time with oxygen saturations between 90-100% was 100%. The apnea index was .4 (nl<1) while the apnea/hypopna index was .4 (nl<1). There were a total of zero central apneas, 0 obstructive hypopneas, 2 obstructive apneas and 0 mixed apneas recorded. Sleepiness scale was 11. (Maybe because he falls asleep in the car and because he may fall asleep if you lay him down in the afternoon?) Toddler/DS snore scale was 4.
Apnea index .4
Apnea/hypopna index .4
Lowest respiratory oxyhemogloblin desaturation 93% with obstructive apnea
Arousal awakening index 10.8
Movement summary
The plm (periodic leg movement) index was 2 (nl<5) The plm arousal index was .4 (nl<5)
Interpretation:
This was a normal study the patient has primary snoring with sleep fragmentation.
Suggestions:
Followup with sleep clinic for further evaluation and management at age 3.
Dr. Ajayi said that he woke up 11 times an hour (sleep fragmentation) when 10 times is normal for a child his age so it's nothing to be concerned about. He said he had adequate NREM for the growth hormone to be released and the highest REM of any DS child he had ever seen (in 11 years).
As for snoring, Jett doesn't snore. He did a little that night because he had been crying for an hour and therefore had some congestion..
Would have liked the REM to be 30%, but I can't complain about 22.3%!
For more info on REM sleep and Ginkgo and how it connects to Down syndrome, see Teresa Cody's blog post: http://changingmindsaboutdownsyndrome.blogspot.com/2011/02/can-sleep-be-as-easy-as-gb.html
Sources
http://science.education.nih.gov/supplements/nih3/sleep/guide/info-sleep.htm
http://changingmindsaboutdownsyndrome.blogspot.com/2011/02/can-sleep-be-as-easy-as-gb.html
http://faculty.washington.edu/chudler/sleep.html
http://www.odec.ca/projects/2004/rich4a0/public_html/information.htm
Related Posts
Jett's Sleep Study: Mommy's Nightmare
Ginkgo: The Hows and Whys for Down Syndrome
Vitamin D3 and Sleep
Link Between Sleep Deprivation & Alzheimer's Risk
Stimulating Growth
DMAE (Dimethylaminoethanol)
Keeping Nasal Passages Clear and Mouths Closed
Ashwagandha
Roobios Tea Protects Brain Against CNS Damage
Nontoxic Bedding
Goji Berries

2 comments:
Great post! I will be talking with my son ENT about sleep Apnea because I want my son strong, in every possible way, when the virus season starts. I will ask if she considered a REM sleep test would be necessary. I know doctors where checking about sleep apnea when he got sick with RSV, but when my son was able to breath on his own again, the lowest oxygen level was 96%. It was also 96% when I took him for an appointment with his Pulmonary doctor and he was having an asthma episode that day. The pulmonary team were happy with his oxygen levels. Thanks for all the info you shared with me about boosting my son's immune system. It has been a great help!
Thank you for this post- I just had a sleep study for my son too with similar results- did Jett end up with treatment? We weren't offered any options since he is so young. Just curious :) Thank you!
Post a Comment